The world in the fight against the coronavirus pandemic. History, figures, facts, problems and forecasts for 2021

2020 turned out to be a difficult year for humanity and will be remembered as one of the most troubling, and for many, tragic periods in its history. The Covid-19 pandemic changed life on the planet, declaring war on human civilization. Throughout the year, countless events occurred that were in one way or another connected to it, and the consequences of these events will be felt for a long time. But, as in any war with its irreparable losses, billionaires during the pandemic earned an amount equivalent to what the G20 countries spent fighting it. The global press is analyzed, figures are cited, and the problems of countries and continents are discussed by Alla Landar, President of the International Association of Funeral Service Professionals (IAFSP), National Member from Ukraine in the World Funeral Directors Federation (FIAT-IFTA), and head of the Kyiv-based private firm “Petro Velykyi.”
Medical science maintains that a pandemic is regarded as an epidemic characterized by the largest-scale spread of an infectious disease across many countries of the world simultaneously—and, moreover, on different continents. Humanity is suffering significant losses due to the lack of collective immunity and effective preventive tools—vaccines—as well as a functional practice and proven methods of treatment. Among the infectious diseases that reached the scale of a pandemic—plague, cholera, or smallpox—the one closest to Covid-19 in scale and nature was the Spanish flu, or “the Spanish Lady,” which lasted from January 1918 to December 1920. Let me remind you: 500 million people fell ill at that time—roughly a quarter of the world’s population. According to various estimates, up to 50 million people worldwide died from the Spanish flu, and according to some modern studies and new sources, even up to 100 million.
This is what the fight against the Spanish flu looked like in Europe.
According to financial experts, billionaires collectively increased their wealth by $3.9 trillion from March to December 2020—an amount equal to what the G20 countries spent on combating Covid-19. This was announced in a report by the international charitable organization Oxfam and was made public by the British public broadcasting company BBC.
At the same time, the world’s ten richest individuals increased their fortunes by $540 billion. According to experts from Oxfam, this sum would have been enough to prevent every person in the world from falling into poverty because of the pandemic, and it would also have covered the cost of vaccines for the entire global population.
The richest eventually came to their senses, as the virus does not choose whom to target based on the size of their wallet, and they began helping the world. According to a report by the Swiss global financial company UBS, 209 billionaires worldwide directed $7.2 billion to charity throughout the year specifically in response to the pandemic.
China: the international team reports
What, above all, marked 2021 in China’s fight against the Covid-19 pandemic? A dozen and a half foreign scientists led by the WHO joined their Chinese colleagues in search of an answer to the question of how the global pandemic began. The vote came after a four-week joint investigation in the city where the first cases were identified—a mission that many hoped would shed some light and provide the long-awaited answers, The Wall Street Journal, one of the largest and most influential U.S. newspapers, reported.
Major international media outlets ran headline after headline on this topic. China resisted the global pressure demanding an investigation, believing it to be an attempt to place blame on the Middle Kingdom. It therefore delayed the mission for months, secured veto rights over participants, and insisted that the investigation’s focus include other countries as well.
In addition, China effectively classified the identities of its own researchers involved in the investigation, exerted pressure on the composition of the international scientific team, and even partially altered the U.S. representation. As a result, what was meant to be a timely and collaborative scientific inquiry moved more slowly, more complicatedly, and less transparently. For this reason, according to American scientists, the world risks never obtaining a definitive answer to the question of the virus’s origins.
The virus had become a politically sensitive issue for Beijing in light of worldwide public outrage. In April 2020, then-U.S. President Donald Trump stated that the virus had likely originated from a laboratory in Wuhan. Chinese officials responded by claiming that it could have spread from the United States. Australia then became the first country to publicly call for an independent investigation, triggering China’s fierce retaliation. Beijing imposed restrictions on imports of Australian wine—something Australian and other foreign officials saw as revenge. After that, disagreements arose among team members, the governments of participating countries, and the WHO…
Throughout all the trips, Chinese scientists and officials accompanied the expert team. According to confidential documents obtained by the reputable New York Times, the WHO agreed that key sections of the investigation concerning the first patients and the role of the seafood market would be written by the Chinese side, while foreign experts would only be allowed to review and supplement the results of their Chinese colleagues.
And finally, China announced that it had shared information collected by more than a thousand Chinese specialists who, since last July, had examined medical records of 76,000 patients from over 200 medical institutions in Wuhan, as well as the results of tests from more than 50,000 animal samples. According to the team members, it became clear to them that Chinese authorities were mostly providing their analysis of the data rather than the raw numbers themselves. They also failed to carry out some of the short-term tasks the scientists had hoped for, including thorough studies of blood samples taken before December 2019 and assembling a definitive list of animals sold at the Huanan market.
WHO experts already in Wuhan
The team of scientists insisted on immediate access to the raw, anonymized data on 76,000 patients—data that, in their view, could have been filtered differently to identify a number closer to a thousand potential earlier Covid-19 infections. The Chinese side refused, the team members said. Chinese participants responded with a study suggesting that the virus may have circulated in other countries in late November and December, and proposed that the WHO investigate whether the pandemic might have originated outside China.
A particularly tense moment emerged after statements from the Wuhan blood bank representatives. Team members demanded blood samples collected before December 2019, which would have been the best way to test the hypothesis that the virus might have spread in China earlier and more widely than presumed. Antibodies could still be detected in frozen samples. The team did, however, secure assurances that the blood samples could be tested later.
The experts visited the Wuhan Institute of Virology and met with Shi Zhengli, the scientist specializing in bat coronaviruses who denies that SARS-CoV-2 leaked from her institute. The team asked why the publicly available virus database had been taken offline. Zhengli said the institute had to remove the database from the internet after roughly 3,000 hacking attempts, according to Dr. Daszak.
Setting aside all the disputes, accusations, and media clashes: in order to present its conclusions to the global community, on February 8 the international team of scientists finally organized a vote expected to shed the first light on the origins of the global pandemic.
The voting addressed four main hypotheses:
- Did the virus pass directly from an animal reservoir to humans?
- Was it transmitted via an intermediate animal?
- Could transmission have occurred through the food chain, especially frozen products?
- What is the likelihood that Covid leaked from a laboratory?
The Wuhan seafood market
Each hypothesis was assessed on a five-point scale: “extremely unlikely,” “unlikely,” “possible,” “likely,” and “extremely likely.” Before the vote, participants presented their arguments for and against each option. The world held its breath…
According to the scientists, the unanimous decision was to classify the laboratory theory as extremely unlikely. At the press conference, Dr. Ben Embarek announced the results. In his words, the most probable hypothesis was that the virus spread from its original animal host—such as a bat—to another animal, and from there to humans. The team would focus its future research on this pathway, and the next priority would be studying whether the virus spread through the food chain, including frozen products. It was also possible, he said, that the virus jumped directly from its original host to humans. It was deemed extremely unlikely that the virus originated from a laboratory, and the team did not recommend further investigation of this hypothesis.
Suspicions of an artificial origin of the infection began spreading actively after the American television channel Fox News reported that the first patient infected with the novel coronavirus had been an employee of the Wuhan Institute of Virology. China’s Foreign Ministry spokesperson Zhao Lijian responded that the theory that SARS-CoV-2 had been engineered in the Wuhan laboratory had no scientific basis.
After the international experts completed their work, Dr. Liang, head of the Chinese team, stated at a press conference that a laboratory origin was impossible because such a virus had not been stored in China at the time.
After leaving Wuhan, some members of the international team issued their own conclusions regarding the laboratories. They said they lacked the authority, expertise, or access to conduct a full examination of the Wuhan Institute of Virology or any other research center. Some spoke about this publicly, others in interviews. Several noted that they were unable to see raw data or original logs of safety protocols, personnel records, experiments, or animal-related data—materials that many other scientists consider essential elements of a complete investigation.
The Wuhan Institute of Virology
Thus, the work of the international commission in Wuhan left much room for reflection. Few realistically expected a comprehensive investigation within just a few months. But the very fact that Beijing did not shut itself off completely and allowed an international team of scientists to work was already a breakthrough and an undeniable positive step.
It is time to look at the current state of affairs with the coronavirus in China. And the picture is as follows. The current Covid-19 statistics as of the end of April: total infected — 90,655; deaths — 4,636, or 5.1%; recovered — 85,691, that is 94.5%; currently ill — 328 people, or 0.4%; among them serious and critical cases — 3. And now the important part: the number of tests performed — 160 million, which is 111,163 per one million people.
As we can see, China continues its successful fight against the coronavirus. It is crucial to avoid new outbreaks among those who have no immunity to Covid-19 and to mitigate the economic consequences of the lockdown. The country faced these challenges earlier than others, and the methods used here may become an example for other nations — either of what should be done, or conversely, of what should never be done under any circumstances. Meanwhile, the vaccination situation in the Middle Kingdom is impressive: population — 1,439,324,000; vaccinations carried out — 253,463,000. Most importantly, China already has its own vaccine — competitive and trusted in the world.
France: unprecedented measures
Doctors at Albert Schweitzer Hospital in Colmar, located in the Haut-Rhin department, became interested in several clinical cases that preceded the Covid-19 epidemic in France. They re-examined several hundred chest X-rays of patients admitted with severe pneumopathies starting in October 2019. One of these patients, hospitalized on November 16, had lesions that clearly indicated Covid-19. Thus, the presence of the novel coronavirus in France was already suspected on that day — however, without biological sample analysis, the hypothesis remained uncertain. The work of French researchers, published in February 2021 in the European Journal of Epidemiology, confirmed these observations. With a high level of evidence, it indicates that SARS-CoV-2 was already spreading in France in November 2019, Le Monde reports.
The researchers, led by Professor Fabrice Carrat, director of the Pierre Louis Institute of Epidemiology and Public Health (National Institute of Health and Medical Research, Sorbonne University), proceeded with exceptional caution. They analyzed 9,144 blood samples taken from participants of the “Constances” cohort — the largest epidemiological cohort monitored in France, numbering over 200,000 people. First, they tested them using a rapid test detecting IgG immunoglobulins against SARS-CoV-2. Since this test is believed to generate false positives, the authors decided to confirm or refute the results using a second, highly specific but more complex test.
Before this, the first confirmed case of Covid-19 in France (detected by PCR) had been a patient hospitalized with severe pneumonia at the end of December 2019 in Seine-Saint-Denis. His frozen samples were re-examined in April 2020 at the initiative of Professors Yves Cohen and Jean-Ralph Zahar of the Avicenne Hospital in Bobigny.
In more than half of the cases, the individuals had either traveled or contacted those who had already fallen ill. One patient had traveled around Asia for two months and returned to France at the beginning of December; another was a physician, which was also a risk factor. Thanks to the large number of blood samples regularly collected from members of the “Constances” cohort since 2018, researchers can now attempt to go even further back in time. The question under examination is whether the virus was present in France already in September — or even August. This view is shared by epidemiologist Marie Zins from the National Institute of Health and Medical Research at Paris University, who is seeking additional funding to conduct further analyses.
Indicators of consistent viral circulation in Europe since November — and even since October — contradict the hypothesis that the epidemic began at the Huanan market in Wuhan, China, in early December 2019. However, they do not cast doubt on established knowledge about the phylogeny or evolutionary development of the virus. All SARS-CoV-2 strains circulating today originate from the virus that appeared at the end of 2019 in China’s Hubei province. This is the opinion of French scientists, as well as the WHO team that completed its work in China.
The French went through several stages in their efforts to overcome the pandemic. Let us recall that when the incidence rate began to rise sharply, France even resorted to extraordinary measures. In addition to unprecedented quarantine restrictions at borders, train stations, airports, and all crowded public places, France revived the long-forgotten wartime term “curfew” and took a radical approach.
Paris during curfew
This sanitary measure proved effective this year, as in the first fifteen departments where the curfew was introduced at 6 p.m., the increase in new cases had already become two to three times lower by January 2 compared with other departments of France.
French epidemiologists are particularly concerned about the spread of the British coronavirus mutation and the new strain from the Republic of South Africa. On this issue, as on everything related to the pandemic, President Emmanuel Macron personally addresses the population regularly on television.
The British variant: will it become dominant?
Let us return to the language of numbers in France. The current Covid-19 statistics are as follows: total infected — 5,592,390; deaths — 104,224 (1.9%); recovered — 4,498,292 (80.4%); currently ill — 989,874 (17.7%); of which serious and critical cases — 5,804. Tests performed — 75,604,728, which is 1,156,160 per million people. With a population of 65,393,000, the number of vaccinated persons is 14,900,784 — 22.79%; fully vaccinated — 6,092,233, or 9.32%. Total vaccinations — 20,969,346.
Italy awaiting its own vaccine
Everyone remembers that the coronavirus began spreading globally from China in December 2019. However, new research has shown that one of the infections occurred already in November 2019. This was reported by Germany’s influential Der Spiegel.
It happened as follows. On November 10, 2019, when a 25-year-old woman in Milan sought medical attention for a skin rash, no one yet knew or suspected anything about a new coronavirus. Doctors took only a skin biopsy. The woman had no other health complaints at the time.
This Milan resident may now have been identified as the first patient of the Covid-19 pandemic. The discovery was made by an international team of scientists coordinated by the University of Milan.
During the pandemic in Italy — so widely reported around the world a year earlier — there were numerous cases where skin irritation was the only symptom. Milanese pathologist Raffaele Gianotti wrote about this in La Repubblica. For that reason, he and his colleagues re-examined atypical skin samples with undetermined diagnoses collected during the last months of 2019.
In the end, the biopsy of the aforementioned 25-year-old woman, taken on November 10, 2019, revealed fragments of viral RNA. She had no other symptoms. She mentioned this when doctors contacted her again. The skin irritation disappeared after five months. A serological test performed in June 2020 showed the presence of coronavirus antibodies, the scientists reported in the British Journal of Dermatology. Let us recall that a serological test (ELISA) detects antibodies in the blood that the immune system produces while fighting a virus. For this, a blood sample must be taken for laboratory analysis. This principle also underlies rapid tests.
It is noteworthy that early media reports mentioned a 55-year-old man from Hubei Province who was said to have been infected as early as mid-November 2019. There was also mention of a shrimp vendor from the infamous large market in Wuhan. However, according to the Italian analysis, their case occurred earlier. As the University of Milan writes, taking into account available international data, the case of the Milan resident is the first evidence of human infection with SARS-CoV-2, Der Spiegel reports.
Everything will be examined — including by WHO experts — but for many in China, not so much for doctors as for politicians, such a turn of events is clearly advantageous.
Doctors together with pharmacologists on the Apennines are determined. Italy promises to present its own coronavirus vaccine in September 2021. This was reported by the ASNA agency.
The corresponding statement was made by the head of the Italian Medicines Agency, Giorgio Palù. According to him, already in September it will be possible to vaccinate several million people.
The Italian company ReiThera is working on the development of the drug. The Ministry of Health has announced that the state will invest significant funds in the company’s research.
Italy has vaccinated more citizens than any other EU member state. Nevertheless, the country is suffering from delays in the delivery of the Pfizer vaccine. Another push toward decisive action was the news from AstraZeneca, which was supposed to meet Italy’s vaccine needs. The company announced that it would deliver fewer doses than planned due to objective reasons: overwhelming demand, the desire to meet everyone’s needs, and yet insufficient production capacity.
What, then, was the pandemic situation in Italy at the end of spring? Total infected — 4,059,821; deaths — 121,738, or 3.0%; recovered — 3,524,194 (86.8%); currently ill — 413,889 (10.2%); serious and critical cases — 2,423; tests performed — 59,552,161, which is 986,175 per million. With a population of 60.387 million, the number of vaccinated individuals is 14,878,628 (24.64%); fully vaccinated — 6,379,737 (10.56%). Total vaccinations — 21,161,899. Essentially, every third person has been vaccinated.
Coronavirus in the USA through the lens of vaccination
Ukrainians traditionally want to know what the situation is overseas regarding the coronavirus pandemic. The information at the beginning of spring was telling: the number of people vaccinated in the USA exceeded the number of those who had been infected. This was reported by Bloomberg.
At the same time, health experts emphasize both the safety and effectiveness of the vaccines. They note that although the vaccines were developed at record speed, they were based on decades of prior research. The vaccines used in the United States have shown no signs of serious side effects among tens of thousands of people, reports Voice of America.
Meanwhile, a winter survey showed that 40 percent of Black Americans across the country said they would not get a coronavirus vaccine. This resistance is stronger than among white Americans, even though the virus disproportionately affects Black communities. It is therefore not surprising that John Curry Jr., pastor of one of the oldest Black church congregations, began encouraging vaccination. He has already been vaccinated and urges his parishioners to follow his example.
Voice of America found that the reason has historical roots. The epicenter of mistrust is the town of Tuskegee. It was once a predominantly Black town where the US government used African American men as “guinea pigs” in a syphilis study. It is therefore unsurprising that even the town’s former mayor, Lousenia Dunn — given the decades-old “Tuskegee Syphilis Study” conducted there — views the Covid-19 vaccine with caution, as well as the government’s promotion of a vaccine developed at record speed, at a time when, in her opinion, the government cannot provide adequate testing or quality medical care in small towns.
These photos from the Tuskegee Syphilis Study are now history.
“I am not getting vaccinated now. That doesn’t mean I’ll never do it. But I know enough to wait until we see all the vaccine-related facts live and in action,” Dunn explains her position.
Therefore, the immunization campaign against the coronavirus began in Tuskegee and other areas of Macon County slowly and hesitantly. The resistance of residents stems from distrust of government promises and decades of failed healthcare programs. Many people in this city of 85,000 have relatives who were subjected to unethical government experiments during the syphilis study.
Other negative news has also emerged. An investigation concluded in Wisconsin: a pharmacist is accused of deliberately removing nearly 60 vials of coronavirus vaccine from a freezer in December, The Washington Post writes.
The Department of Justice issued a firm statement: it will prosecute anyone — especially medical workers — who intentionally destroys vaccines. The hospital where the 46-year-old suspect, Steven Brandenburg, worked had to discard nearly 600 doses. Even the FBI joined the investigation.
Colleagues of the suspect said he was influenced by conspiracy theories and believed the vaccine could harm people. The suspect agreed to plead guilty to tampering with vaccines, but fortunately this was an isolated case.
The newly elected president immediately joined the fight against the coronavirus pandemic. Joe Biden is ready to consider adjustments to his proposed $1.9 trillion pandemic relief package so that the funds go to Americans who need them most.
Brian Deese, director of the National Economic Council, told CNN that the proposal “matches the economic crisis we face” and that the president is “unyielding when it comes to the speed with which we need to act,” including responding to the economic slowdown, insufficiently rapid vaccination distribution nationwide, and the steady rise in Covid-19 deaths at the beginning of the year in the United States.
Beginning February 1, everyone in the United States will be required to wear a mask while boarding, disembarking, and traveling on any conveyance entering or operating within the United States, as well as in any transportation hub (terminal, station, etc.) that facilitates travel within the country.
Recently it became known that Ukrainian doctors in the United States are debunking myths about Covid-19 vaccines. More details can be found in the report: https://ukrainian.voanews.com/a/5757201.html
In New York, the infection curve has begun to decline. In view of the easing of the pandemic, New York authorities announced that restaurants in Manhattan and other boroughs of the city are allowed to partially resume indoor service.
Meanwhile, scientists at the Ohio State University Medical Center have identified two new coronavirus variants in the United States. They likely emerged within the country itself. The report states that one of them is similar to the so-called “British” variant. The first of the two was discovered in a patient from Ohio. Researchers are studying how widespread it may be.
The second variant, which contains three mutations, was detected in Columbus. It is more contagious than earlier known strains. And the first case of infection with the “British” variant in the United States was confirmed back on December 29 in the state of Colorado.
As already reported, at the end of 2020 a new coronavirus variant was identified in the United Kingdom — designated VOC 202012/01. According to research, it is 50–74% (depending on the estimate) more dangerous than the SARS-CoV-2 virus that causes Covid-19. To date, VOC 202012/01 has already been detected in about thirty countries worldwide.
Let us finally look at U.S. statistics at the beginning of May: total infected — 33,274,659; deaths — 592,409 (1.8%); recovered — 25,966,389 (78.0%); currently ill — 6,715,861 (20.2%); serious and critical cases — 9,451; tests performed — 451,246,395, or 1,356,591 per million. And now vaccination: with a population of 332.627 million — vaccinated 147,517,734 (44.35%); fully vaccinated — 105,523,520 (31.72%). Total vaccinations — 246,780,203. It is difficult even to imagine, let alone comment on such figures.
The virus in forecasts by Austrian scientists
For many years virologists have been warning about the danger of a viral pandemic, insisting that it must finally be taken seriously, writes the Austrian publication Der Standard. “The start of a new pandemic is only a matter of time. We simply do not know where and how it will happen,” says epidemiologist Syra Madad. As we can see, the researcher at that time did not yet know how quickly everything could unfold.
Der Standard met with another expert roughly a year after the first reports of the emergence of the respiratory disease Covid-19. Dennis Carroll, a virologist who leads the global “Global Virome Project” — aimed at sequencing, or systematically cataloguing, the maximum number of viruses that may pose a threat.
Carroll spoke about more than 600,000 zoonotic viruses. Zoonoses are natural-focal infections found in animals but capable of being transmitted to humans. Viruses with zoonotic potential — living in wild animals as in a kind of reservoir — can, under certain circumstances and through an intermediate host such as poultry or livestock, theoretically be transmitted to humans. According to his estimates, there are 1.7 million different viruses. Given the many unknowns in this field, the researcher refers to this as the “dark matter” of viruses.
Austrian virologist Florian Krammer, an expert at the Mount Sinai Medical Center in New York, also believes the danger is significant. “We should have adapted to many types of viruses over many years already, but instead we wait. It is now obvious that this is a mistake,” he says. Along with coronaviruses — around 4,000 of which are potentially dangerous — the greatest concerns are paramyxoviruses, which include the pathogens of mumps, measles, and Nipah virus. The latter recently caused an outbreak in Bangladesh. It is transmitted from fruit bats to livestock and then to humans.
Paramyxovirus under a microscope
The pathogen spreads through aerosols and can lead to fatal inflammation of the brain membranes. A third group of viruses capable of causing an epidemic (a limited outbreak) or even a pandemic (disease spread worldwide) are orthomyxoviruses, which include influenza viruses. Norbert Nowotny, a virologist at the University of Veterinary Medicine in Vienna, points to another danger: influenza viruses are capable of exchanging entire segments of their segmented genome with other viruses, potentially creating a new pathogen to which humans have no immunity.
Orthomyxoviruses under a microscope
According to Florian Krammer, the intervals between outbreaks of new infectious diseases have shortened in recent years. The head of the Global Virome Project, Dennis Carroll, identifies the main reasons, in his view: the world’s population has increased sharply in a short period of time. Today it is about 7.8 billion people, compared with 1.6 billion in 1900. Land use has expanded; the natural habitats of hundreds of wild species have been destroyed. Humans use nature for their own purposes and come into contact with animals — whose viruses can be dangerous — more and more often.
Scientists have long warned about this problem. In October 2018, researchers from the Peter Doherty Institute for Infection and Immunity at the University of Melbourne warned in the journal Frontiers in Cellular and Infection Microbiology about the danger of a second Spanish flu. Recall that the original “Spanish flu” killed about 50 million people. In 2019, Chinese scientists demonstrated in the journal Viruses how dangerous the connection between bats (likely reservoirs of SARS-CoV-2) and coronaviruses can be.
Carroll sees only one way to prevent the danger of future pandemics: “We must fundamentally change our attitude toward the environment and nature, and adjust our way of life.” Krammer agrees, but does not believe this will happen. He sees more hope in preparing consistent measures: alongside a global map of virus prevalence, this could take the form of a global pandemic-response plan that most countries would have to follow.
Austria also experienced a lockdown due to the spread of the new British variant. The newly identified strain is more contagious, so Austria has taken decisive safety measures.
Coronavirus in Austria at the beginning of May: infected — 624,595; deaths — 10,291 (1.6%); critical cases — 459; tests performed — 32,895,293, or 3,635,018 per million. With a population of 9.049 million, the number of vaccinated individuals is 2,360,698 (26.09%); fully vaccinated — 864,971 (9.56%); total vaccinations — 3,225,441.
What, then, is the solution according to Austrian scientists? A much stronger implementation of measures to contain the pandemic is needed. Stefan Thurner, president of the Complexity Science Hub (CSH) in Vienna, criticizes the approach in which the only working tool remains the lockdown. According to him, this tool originates from the Middle Ages and was introduced by Pope Alexander VII to protect people from the plague.
Today, he says, it urgently needs to be supplemented with digital solutions for the rapid identification of infected individuals. The researcher calls for further digitalization of the healthcare system. Otherwise, it will be impossible to coordinate the necessary logistics, and the required speed of response and localization will continue to be insufficient.
Meanwhile, pharmaceutical efforts must focus on antiviral medications to ensure constant readiness to fight epidemics, since no one can predict what humanity will face next.
Funerals during the coronavirus pandemic
Many questions related to the spread of Covid-19 over the past year and a half have concerned people. Among the first: how are farewells to those who died from the coronavirus conducted around the world?
Let us recall how it all began. At the start of the pandemic, disinfectants and protective equipment suddenly became scarce, causing difficulties even for funeral homes. Managers of many such companies feared they would soon be unable to perform their work, wrote the German magazine Der Spiegel in spring 2020 during the peak of the first wave.
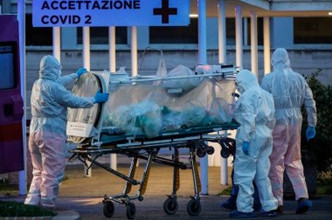
The world watched in horror the news footage from Italy, where coffins were transported to crematoria on military trucks. The provinces of Bergamo and Brescia felt the blow of the pandemic especially strongly, as the local warm and humid climate became an ally of the virus.
In Spain and the United States, hundreds of people died daily, and funeral services in Germany braced for similar scenarios, as Munich and Frankfurt airports — where three planes landed or took off every 3–5 minutes — processed hundreds of thousands of passengers daily, until they eventually shut down.
Funeral homes across Germany ordered coffins and body bags, mostly from Eastern Europe. Many changed their usual operating procedures to protect their employees. No one knew the correct course of action. In Hamburg, for example, one of the two crematoria was initially closed to concentrate cremation in a single location. Employees of the other crematorium were kept in reserve in case a mass outbreak affected their colleagues. Contact with clients, relatives, and loved ones of the deceased was minimized.
German journalist Michael Frelingsdorf recalls: “When funeral home employees wash, dress, and place the deceased in coffins, they are in contact with those who may have died from the coronavirus. Although the dead do not release viruses into the environment by coughing, they do release biological fluids, and gases escape from the lungs and intestines — especially when the body is lifted into the coffin. Therefore, funeral home employees generally had to protect themselves from the dangerous virus on their own.”
If the death certificate contained a medical statement that the deceased had been infected with the coronavirus, additional precautions were taken: the body was placed in a special protective cover or wrapped in materials soaked with disinfectants. In the early stage, those who died from coronavirus were additionally fitted with mouth-and-nose masks moistened with special chemicals.
Why did German funeral homes find themselves in such difficult conditions during the first wave of the pandemic? Unlike doctors and medical staff — who were supplied with protective gear by medical associations and health authorities — funeral homes in most federal states were not classified as organizations belonging to the pandemic-response system, and therefore did not receive the necessary protective equipment. For this reason, funeral homes had to resolve all issues concerning disinfectants, protective clothing, and personal protection on their own.
At the onset of the pandemic, the problem became so serious that some funeral homes and agencies were on the verge of halting their work altogether. Der Spiegel reported that the Federal Association of German Funeral Directors in Düsseldorf received hundreds of calls from concerned members, recalls the association’s general secretary, Stefan Neuser. He therefore raised this issue directly with the Minister of Health, Jens Spahn. Additional protection was urgently needed because there was a significant risk: among the deceased, there were likely many with undetected viral infections. That is, if someone died of coronavirus in a hospital, the information in the death certificate was generally reliable. But for those who died in nursing homes, certainty was far lower. Thus, what could not be reliably established in the case of the living was unlikely to work with the dead — and above all, there was practically no coronavirus testing, Der Spiegel notes.
The reputable Deutsche Welle described the situation in German crematoria during the first wave. The manager of the crematorium in Döbeln, in the federal state of Saxony, Herold Münster, long hesitated whether to show journalists what was happening in his facility. He always believed that the funeral ceremony and everything associated with it should be worthy of the memory of the deceased. Especially in those days, he did not want to alarm people, but given the worsening daily situation, he decided to share everything with the press.
Herold opened the doors of the crematorium building and showed where farewell ceremonies had usually taken place, pointing to a room designed for 90 people. But now, in the space where relatives had typically sat during ceremonies, countless wooden coffins stood. They were stacked on top of each other, and some were marked: “coronavirus.”
The crematorium had reached its limits, and the mourning room had gradually been converted into a staging area for bodies awaiting cremation. Farewell ceremonies had to be abandoned entirely. In the courtyard, a trailer with an additional refrigeration unit was installed to store bodies before cremation. And this situation was common throughout Europe: funeral homes sought to create reserve storage as quickly as possible. In Saxony alone, mortality rose by 109 percent.
Italy, the first EU state to face a large-scale outbreak, began by banning funeral Masses in all churches — a practice that had long been the only dignified form of farewell in Catholic Italy. Clergy tried to reassure families and promised to hold a memorial Mass for every deceased person once the epidemiological situation improved. Nevertheless, families were allowed to invite a priest for a brief prayer.
The Italian alternative became short funerals, without the traditional procession from home to cemetery. Everyone present had to maintain distance, and all physical contact — including handshakes and expressions of sympathy — was forbidden.
What do Italians say about this? The coronavirus strikes the sick twice: first, the infected die in isolation, far from their loved ones, and then they take their final journey accompanied by strangers. Online funerals became more common. Patients passed away in isolated hospital rooms into which relatives were strictly forbidden to enter. The most doctors could do was connect those nearing death with their families via Skype, allowing loved ones a final farewell.
From a logistical standpoint, the Italian funeral sector — especially in the north — experienced enormous strain: the large number of deaths created backlogs in burials and cremations. One only has to recall the horrifying scenes in Bergamo: rows of coffins lined up inside churches. An entire generation died within a few weeks. Since local cemeteries and crematoria could not cope with the numbers, the military had to transport bodies to neighboring provinces. Similar situations occurred in Emilia-Romagna. Matters were worsened by the fact that many funeral homes were themselves quarantined, and those that remained open soon ran out of money for protective equipment.
DW recalls a case in the UK: the family of an elderly man who died from coronavirus could not organize a funeral because all of them were in quarantine. The head of the family returned from a two-week trip to northern Italy, and three days later fell ill. The coronavirus was not diagnosed at once, as symptoms were attributed to existing arthritis and heart disease. After several days of isolation, the elderly man died, and his family had to remain in quarantine. Such cases were increasing daily in Britain.
The Irish Association of Funeral Directors, which unites 342 funeral homes, issued recommendations at the first signs of the pandemic. The leadership insisted that all those who died from Covid-19 be immediately transported either to the crematorium or the cemetery; all ceremonies involving relatives, friends, or colleagues were to be postponed. Funeral vehicles had to be disinfected after each service, and all communication with families was to occur by phone only. Relatives were not allowed into funeral facilities or morgues. Church services and memorial gatherings were to be avoided. The association also required that bodies of Covid-19 victims be transported only in sealed body bags.
Following Italy, Spain was struck hard by the pandemic. Burying coronavirus victims became increasingly difficult. In the early stage, some funeral homes simply refused to handle Covid-19 bodies to prevent infection among attendees. Others minimized contact with bodies: they used thick burial shrouds, immediately sealed the coffin, and kept it closed throughout the ceremony. Drivers of hearses and all funeral workers wore protective suits. This drastic change came after a report that in the city of Vitoria, more than 60 relatives and friends were infected at a single funeral — a shocking revelation.
In Madrid, a protocol originally developed in 1997 was activated for deaths involving diseases dangerous to funeral personnel and the public. The document required complete disinfection of all premises associated with the deceased and their relatives.
What about France? According to the Federation of Funeral Services, French law forbids all body preservation procedures for those who died from infectious coronavirus. The deceased must be placed immediately into a closed coffin. However, there were no special instructions from the Ministry of the Interior regarding the timing or location of burials, nor the format of ceremonies.
Japan, Asia’s most cautious nation, did not ban funeral rites or memorial services, but urged citizens to avoid large gatherings. Funeral ceremonies were limited to incense offerings according to Buddhist custom, with memorial meals cancelled. People came in disposable masks and stood at safe distances instead of sitting close together as tradition dictates.
And finally, China. News from China rivaled only Italy in quantity and intensity, so there is little need to repeat them. China introduced radical measures immediately, even amending the criminal code with a provision on intentional coronavirus transmission.
In Beijing, both funerals and weddings were banned. Funerals were prohibited because they typically gathered large crowds. Similarly, weddings were suspended. In China — regarded as the epicenter of the global spread — the body of the deceased is not shown to the family. Ceremonies are shortened drastically. In some cities, only one funeral home is allowed to handle Covid-19 victims, supported fully by the state to minimize contact with the infected deceased. Traditionally, cremated remains were stored until the Qingming Festival in March–April. This, too, was cancelled. The annual Tomb Sweeping Festival was held online.
In South Korea, a country known for demographic challenges, the government urged families to cremate the deceased first and only afterward hold small memorial ceremonies.
In Iranian society, at a man's funeral people usually greet each other with hugs according to Muslim tradition. However, current restrictions have deprived everyone of this long-standing custom. Farewells in complete solitude. Iran already has thousands of people who have gone through such experiences, calling it “mourning at a distance.” As a result, few people now attend funerals not only of those who died from the virus, but also of those who passed away for other reasons. “When you cannot mourn your loved ones, you cannot believe in their death,” they say in Iran.
A few words about the Vatican. Pope Francis closed St. Peter’s Basilica and the adjacent square in the Vatican due to the coronavirus. He traditionally delivers his addresses from the balcony of the basilica. Religious services in Roman churches were decided to be held without public participation. Churches were closed as well, so Masses are conducted online.
In friendly Georgia, approaching the coffin is prohibited. Bodies must be buried within 72 hours after the confirmation of death. The deceased is buried wrapped in hermetically sealed plastic. A rather unexpected piece of news is that the bodies of Georgian citizens who died from coronavirus in other countries are buried in those same countries.
According to the recommendations of the World Health Organization, as few people as possible should attend funerals of coronavirus victims. The body of the deceased should, if possible, not be transported from one locality to another. As of early May, more than 1.5 million people worldwide have been infected with the coronavirus. Therefore, the most important safety measure for humanity in 2021 remains vaccination, the study of new strains, and the systematic documentation not only of each regional outbreak of the pandemic but also of each individual case. The development of new vaccines also remains relevant, as each existing one still has flaws and limitations.
The recommendations for everyone remain unchanged. If Covid-19 transmission is registered in your area, follow simple safety rules: keep a safe distance from others, wear a mask, ventilate rooms well, avoid crowded places, wash your hands, and cover your nose and mouth with your elbow or a tissue when coughing or sneezing. WHO recommendations are widely available online on numerous websites and translated into most of the world’s languages.
At the same time, it is important to monitor the recommendations for each country, region, locality, and even workplace from your own Ministry of Health and national sanitary authorities.
In addition to vaccination and treatment methods, new problematic issues have arisen that scientists will have to work on in the coming years. They are related to rehabilitation due to complications and consequences after the illness: muscle pain, constant fatigue, and even psychological problems. Those who suffered a severe form of Covid-19 may experience aftereffects even six months after infection. Life dictates new tasks for researchers, while the general population must continue following all recommendations, because it is better to learn from someone else’s sad experience than to face your own.